What is an At-Home Sleep Test and How Does It Work?
An at-home sleep test is a convenient diagnostic tool you wear overnight in your own bed to detect breathing-related sleep disorders, particularly obstructive sleep apnea. You receive a small monitoring device that tracks vital signs while you sleep naturally at home.
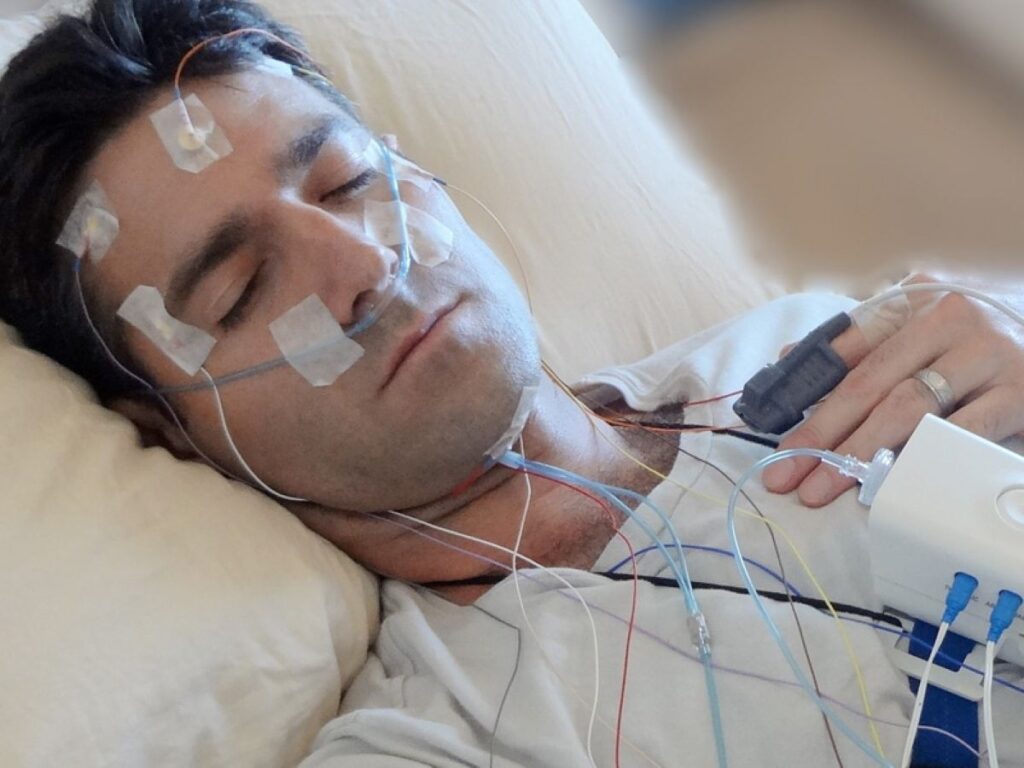
The test uses compact sensors positioned on specific body areas to gather critical data during a home sleep study Sydney patients can complete comfortably in their own environment. A finger sensor clips onto your fingertip like a pulse oximeter, measuring oxygen saturation levels and heart rate throughout the night. Alternatively, some devices use chest sensors that attach with adhesive strips to monitor breathing patterns and detect interruptions in airflow.
What Data Gets Collected During Testing?
The sensors capture four primary metrics:
- Breathing patterns – tracks respiratory rate and identifies pauses or irregularities
- Oxygen levels – monitors blood oxygen saturation to detect drops during sleep
- Heart rate – records cardiovascular responses to breathing events
- Snoring – detects frequency and intensity of snoring episodes
How Does the Data Reach Sleep Specialists?
Modern at-home sleep tests connect wirelessly to smartphone apps that automatically upload your sleep monitoring data to a secure portal. A board-certified sleep specialist reviews the information, analyzing patterns that indicate sleep-disordered breathing. The entire process typically takes 1-3 business days from data submission to receiving your results and interpretation.
The technology eliminates the need for overnight hospital stays while providing clinically valuable insights about your nighttime breathing and oxygen stability.
Why Should They Consider Taking an At-Home Sleep Test?
At-home sleep tests offer significant cost savings compared to in-lab studies, often costing 50-70% less while providing accurate results for obstructive sleep apnea detection. The comfort of sleeping in your own bed eliminates the stress and unfamiliarity that can affect sleep quality during traditional polysomnography.
Convenience stands as a major advantage. You avoid traveling to a sleep clinic, spending the night in an unfamiliar room with multiple wires attached to your body, and disrupting your normal sleep routine. The test fits seamlessly into your regular bedtime schedule.
Wait times for in-lab sleep studies can stretch from several weeks to months depending on your location and insurance requirements. At-home testing typically arrives within days of prescription, allowing you to begin the diagnostic process almost immediately. This speed matters when sleep apnea symptoms are affecting your daily life, work performance, or overall health.
Early diagnosis through accessible at-home testing prevents the progression of untreated sleep apnea, which links to serious health complications:
- High blood pressure and cardiovascular disease
- Type 2 diabetes
- Stroke risk
- Daytime fatigue leading to accidents
- Cognitive decline and memory problems
The affordability of at-home tests removes financial barriers that might otherwise delay diagnosis. Many insurance plans cover these tests with lower copays than in-lab studies, making sleep health accessible to more people who suspect they have breathing-related sleep disorders.
Starting treatment earlier based on prompt test results leads to faster improvement in sleep quality, energy levels, and reduced health risks. The sooner you identify sleep apnea, the sooner you can implement effective treatments that restore restorative sleep patterns.
Who is the Ideal Candidate for an At-Home Sleep Test?
At-home sleep tests work best for adults showing clear obstructive sleep apnea symptoms who fall into moderate risk or high-risk categories. Your healthcare provider will likely recommend this testing if you exhibit multiple warning signs that suggest breathing disruptions during sleep.
Heavy Snorers
Heavy snorers represent prime candidates, particularly when their snoring is loud enough to disturb partners or occurs nightly. The snoring pattern matters too—irregular snoring interrupted by gasping or choking sounds indicates potential airway blockages that warrant investigation.
Overweight Individuals
Overweight individuals face elevated risk due to excess tissue around the neck and throat that can obstruct airways during sleep. Body mass index (BMI) over 30 significantly increases the likelihood of developing sleep apnea, making at-home testing a practical screening tool for this population.
Hypertension Patients
People with hypertension often receive recommendations for sleep testing since untreated sleep apnea contributes to high blood pressure. The relationship works both ways—those with resistant hypertension that doesn’t respond well to medication frequently have undiagnosed sleep apnea.
Healthcare Provider Recommendations
Healthcare providers typically suggest at-home testing when patients report:
- Excessive daytime sleepiness despite seemingly adequate sleep hours
- Morning headaches that fade as the day progresses
- Difficulty concentrating or memory problems
- Witnessed breathing pauses during sleep reported by bed partners
- Waking up gasping or choking
- Frequent nighttime urination
Type 2 Diabetes Patients
Type 2 diabetes patients also qualify as strong candidates since sleep apnea and diabetes share bidirectional relationships. Sleep disruptions affect blood sugar regulation, while metabolic issues can worsen breathing problems during sleep.
Atrial Fibrillation and Heart Rhythm Abnormalities
Your doctor may prioritize at-home testing if you have atrial fibrillation or other heart rhythm abnormalities, as oxygen deprivation from sleep apnea strains cardiovascular function. Men over 40 and postmenopausal women face naturally higher risk levels that justify proactive screening.
Anatomical Features
Certain anatomical features increase candidacy: a thick neck (over 17 inches for men, 16 inches for women), recessed chin, large tonsils, or narrow airway. These physical characteristics create structural vulnerabilities for airway collapse during sleep.
What are the Limitations of At-Home Sleep Tests?
At-home sleep tests may miss mild OSA cases because they use fewer sensors than comprehensive lab studies. The simplified monitoring setup tracks basic breathing metrics but lacks the sensitivity to detect subtle disruptions in sleep patterns. Someone with mild sleep apnea experiencing 5-14 breathing interruptions per hour might receive a negative result, leaving their condition undiagnosed and untreated.
Sensor errors occur more frequently with at-home testing compared to supervised lab environments. The devices rely on proper placement and secure attachment throughout the night. If a finger sensor slips off during sleep or a chest band loosens, the recording becomes incomplete or inaccurate. Technical issues like low battery life, poor Bluetooth connectivity, or user error in setup can compromise data quality.
The limited scope of at-home sleep tests means they exclusively target breathing-related sleep disorders. These tests measure:
- Airflow through nasal passages
- Blood oxygen saturation levels
- Heart rate variability
- Chest and abdominal movement
- Snoring intensity and frequency
Conditions beyond OSA remain undetectable through at-home testing. Narcolepsy, which causes excessive daytime sleepiness and sudden sleep attacks, requires brain wave monitoring unavailable in home devices. Periodic limb movement disorder, restless leg syndrome, REM sleep behavior disorder, and central sleep apnea need the comprehensive data collection that only in-lab polysomnography provides.
The absence of video monitoring and direct observation means unusual sleep behaviors go unnoticed. Sleep technicians in lab settings can document sleepwalking, teeth grinding, or abnormal movements that might explain poor sleep quality. Home tests capture numerical data without the contextual information that visual observation provides.
See Also : Understanding the Adelaide Sleep Study Cost and What It Covers
How Can Results from an At-Home Sleep Test Improve Their Sleep Quality?
Positive test results provide a clear diagnosis that opens the door to targeted interventions designed specifically for their condition. When obstructive sleep apnea is confirmed, sleep specialists develop personalized treatment planning that addresses the severity and unique characteristics of their breathing disruptions during sleep.
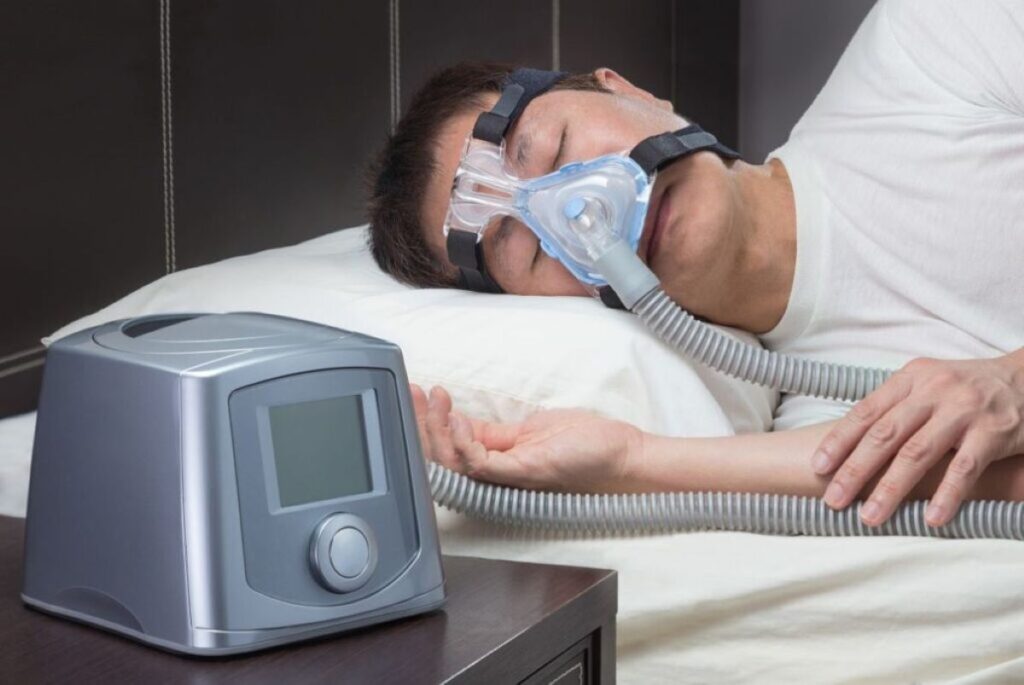
CPAP Therapy: The Most Common Treatment for OSA
CPAP therapy stands as the most common and effective treatment for moderate to severe OSA. This device delivers continuous positive airway pressure through a mask, keeping airways open throughout the night. Most patients experience immediate improvements in sleep quality, daytime alertness, and energy levels within the first few weeks of consistent use.
Behavioral Changes: Important Additions to Treatment Plans
Behavioral changes form another critical component of treatment plans. These changes could include:
- Weight management strategies can significantly reduce OSA severity, as excess weight around the neck contributes to airway collapse.
- Positional therapy helps those whose apnea worsens when sleeping on their back by training them to sleep on their side.
- Alcohol avoidance before bedtime prevents throat muscle relaxation that worsens breathing obstruction.
- Sleep schedule optimization ensures adequate rest periods and consistent sleep-wake times.
It’s worth noting that some of these behavioral changes are not just limited to adults but can also apply to children. For instance, weight management and optimizing sleep schedules are crucial for children as well, especially if they are facing issues like behavioral disorders which could be exacerbated by poor sleep quality.
Dental Appliances: Alternatives for Mild Cases or CPAP Intolerance
Dental appliances offer an alternative for mild to moderate cases or for those who cannot tolerate CPAP. These custom-fitted devices reposition the jaw and tongue to maintain open airways during sleep. They work particularly well for patients with specific anatomical features contributing to their apnea.
Surgical Interventions: Considerations When Other Treatments Fail
Surgical interventions become considerations when other treatments prove ineffective or when structural abnormalities require correction. Procedures range from removing excess tissue in the throat to repositioning the jaw for better airway alignment.
Addressing diagnosed sleep apnea through any of these treatment approaches directly improves sleep quality by:
- Eliminating frequent breathing interruptions that fragment sleep cycles
- Restoring oxygen levels throughout the night
- Reducing strain on the cardiovascular system
- Decreasing snoring that disrupts both the patient and their bed partner
- Enabling deeper, more restorative sleep stages
The ripple effects extend beyond nighttime rest. Patients typically report reduced daytime sleepiness, improved concentration, better mood regulation, and decreased risk of serious health complications like heart disease, stroke, and diabetes. Their relationships often improve as snoring diminishes and irritability decreases
What Steps Should They Take After Receiving Their Test Results?
Positive Results: Immediate Action Required
Positive results require immediate specialist consultation to begin treatment. A sleep specialist will review the data, confirm the diagnosis, and create a personalized treatment plan based on the severity of sleep apnea detected.
The follow-up care process typically includes:
- Treatment initiation: Starting CPAP therapy or other prescribed interventions within 2-4 weeks
- Equipment fitting: Proper mask selection and machine calibration for CPAP users
- Follow-up appointments: Scheduled check-ins to monitor treatment effectiveness and adjust settings
- Lifestyle counseling: Guidance on weight management, sleep position changes, and avoiding alcohol before bed
Negative Results: Don’t Ignore Ongoing Symptoms
Negative results don’t always mean perfect sleep health. If symptoms persist despite a negative test, further investigations may be necessary. The at-home test might have missed mild sleep apnea or other sleep disorders entirely.
Patients with negative results but ongoing symptoms should:
- Schedule a specialist consultation to discuss persistent issues like daytime fatigue or morning headaches
- Consider comprehensive in-lab polysomnography to detect non-breathing-related disorders
- Keep a detailed sleep diary documenting symptoms, sleep patterns, and daytime impairment
- Explore other potential causes such as insomnia, restless leg syndrome, or circadian rhythm disorders
Act Promptly for Better Sleep Quality
Take Our Simple At-Home Sleep Test to Improve Your Sleep Quality by acting on results promptly. Delaying treatment allows sleep apnea to worsen and increases risks of cardiovascular problems, diabetes, and cognitive decline.
Insurance coverage often requires timely follow-up, so contacting a sleep specialist within 30 days of receiving results helps ensure benefits remain active. Many sleep centers offer telehealth consultations for initial discussions about test findings.

